17 May 2013
How Do Neurons Recognize Each Other at Synapses?
In order to carry out the complex physical and mental functions required in daily life, the many neural circuits that allow communication between different parts of the brain must be properly connected. While electrical impulses transmit information along neuron fibers, communication across synapses, the junctions where two neurons meet to form these neural circuits, occurs through the release and uptake of chemicals called neurotransmitters. Neurotransmitters are first collected in vesicles, or tiny bubbles within the ‘presynaptic’ neuron, then released into the synapse, and finally collected by the neighboring, or ‘postsynaptic’, neuron to complete the chemical transmission. Until recently researchers were unsure as to how some neurons recognize each other to create the correct synaptic connections that form these vital neural circuits.
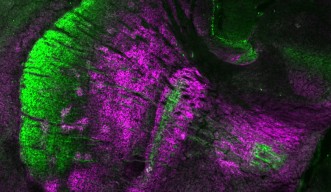
In a paper to be published in the June 5 issue of Neuron, Professor Tadashi Yamamoto and Dr. Naosuke Hoshina of the Cell Signal Unit and colleagues have identified the protein that regulates the assembly of synapses in neural circuits that connect the basal ganglia and the cerebral cortex. Specifically, the researchers found that neurons in these circuits recognized each other because they both expressed the protein PCDH17. In addition to facilitating the proper formation of synapses in the cortico-basal ganglia circuits, PCDH17 was also found to indirectly regulate the assembly of neurotransmitter-filled vesicles in the presynaptic neuron, as vesicle assembly is triggered after two neurons form a synaptic connection.
Communication between the basal ganglia and the cerebral cortex is vital for carrying out brain functions associated with movement, learning, emotion and motivation. Dysfunctions along these circuits are known to lead to physical and mental diseases, such as Parkinson’s disease, obsessive-compulsive disorder, schizophrenia and depression. In fact, the OIST researchers and their co-authors also found that when PCDH17 was absent, mice exhibited anti-depressive behaviors, such as a higher resistance to stress, suggesting a malfunction in this protein may play a role in causing depression.
“The brain is an incredibly complex organ,” says Yamamoto. “By understanding the precise mechanisms that allow for the healthy functioning of cortico-basal ganglia circuits, we’re one step closer to understanding how diseases such as depression can be better treated.”
Research Unit
Submit a press inquiry