10 December 2014
Accelerating Particles into Medicine
Distinguished Professor Hirotaka Sugawara has opened the new Advanced Medical Instrumentation Unit at the Okinawa Institute of Science and Technology Graduate University. The unit will apply particle and nuclear physics research to improve medical technology. Sugawara describes two projects to start the unit: a new cancer therapy and a more precise brain imaging technique.
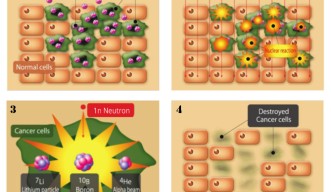
“Okinawa Prefecture is trying to make a facility in West Futenma in Ginowan City for heavy ion cancer therapy,” Sugawara says, explaining the new idea that he envisions replacing chemotherapy. One heavy ion cancer therapy involves adding boron to the body, then using a neutron beam to strike the boron. The boron releases cancer-killing alpha particles, but only within a range of one millimeter. The method increases the precision of cancer therapy, minimizing damage to healthy cells. But in order to produce the most effective neutron beam, he needs an accelerator.
“So far, people have been using neutrons from nuclear reactors,” Sugawara says. Some researchers create neutron beams from the neutrons that come off of the reactors, then apply them to cancer therapy experiments. But this is not a common practice. “Nuclear reactors are not everywhere,” says Sugawara, “and the neutron means they produce are not strong enough.” Sugawara says his unit will work both on developing smaller, more affordable accelerators and on improving the cancer therapy. “We will be working together with Ryukyu University Medical School in addition to other medical schools in Japan,” says Sugawara. “Hopefully some other medical schools in the US and other countries will join.”
Sugawara also has his eye on imaging techniques, especially to improve cancer visualization. Current methods, such as PET, create images by first injecting fluoride into the area. The fluoride emits a positron, which moves a millimeter and then releases two gamma rays. The imaging system measures the gamma rays emitted, but because of the positron’s movement, any measurement could be one millimeter off. This limits the resolution of any image to one millimeter. This is a problem, because cells are usually measured in micrometers, three orders of magnitude smaller than one millimeter.
“The mechanism of cancer is not well known,” Sugawara says. He’s been following research on the cancer stem cell hypothesis, which claims that cancer cells can only come from one type of cell in the human body: somatic stem cells. Kill the somatic stem cells and the tumor should stop growing. But in order to test this hypothesis, let alone treat patients, doctors need a better imaging method to measure tumor growth and see what’s happening inside the body. With precise imaging to target stem cells, radiation therapy could even be capable of treating cancer after metastasis, or after it has spread to other organs.
Sugawara says that by replacing the fluoride with a particular sodium isotope, he can emit gamma rays without the positron throwing off the measurements, thus increasing image resolution. “We want to improve this resolution to the micrometer level,” Sugawara says. “It’s not an easy thing to do; it’s a completely different technology.”
Sugawara is excited to embark on an interdisciplinary study area. “We have to work with medical researchers, biologists, engineers, and physicists,” he says. “Everyone must get together, and by doing so, we may come up with very interesting new ideas.”
by Poncie Rutsch